


Meet Debunked:
For all the bumps in life




Meet Debunked:
Pelvic health is essential for overall well-being as the pelvic floor muscles play a critical role in:
As Peinado-Molina et al. (2023) state, strong pelvic floor muscles are essential for supporting your spine, preventing incontinence, and enhancing sexual health. Moreover, pelvic floor health is crucial during pregnancy and postpartum recovery, as it helps prevent pelvic organ prolapse, perineal tearing, and incontinence. Furthermore, optimizing your pelvic health can lead to a smoother recovery overall.
Additionally, addressing pelvic health issues can improve mental health by alleviating anxiety and social isolation caused by conditions such as incontinence or pelvic pain (Peinado-Molina et al., 2023). Prioritizing your pelvic health can lead to a healthier, more confident, and fulfilling life.
However, even though we recognize the importance of pelvic health for overall well-being, it remains shrouded in shame, misconceptions, and myths. Understanding the truths about pelvic health can lead to better care and treatment for those experiencing pelvic-health-related issues. Now, let’s debunk five common myths about pelvic health!
Myth: Pelvic health concerns exclusively affect women or those assigned female at birth.
Fact: Men and children can also experience pelvic health issues, including pelvic pain, incontinence, and pelvic floor dysfunction including long term hip and low back pain!
Everyone has a pelvis! And that means, pelvic health can affect every body, at any age, and all genders.
While it’s true pelvic health issues are often associated with women or individuals assigned female at birth (Davis & Kumar, 2003), because they experience childbirth and menopause, it doesn’t mean men and children are immune. Men can suffer from conditions like persistent pelvic pain, erectile dysfunction, prostatitis, and incontinence.
Even children can experience pelvic floor dysfunction such as constipation, incontinence, bed wetting, and core-related conditions. Recognizing pelvic health is not gender or age-specific helps in addressing and treating these conditions across the lifespan.
Myth: Kegels are the only type of pelvic floor exercise.
Fact: Pelvic floor exercises consist of more than Kegels (and in some instances, Kegels may worsen a condition!)
Kegels are exercises designed to strengthen the pelvic floor muscles, which support the bladder, bowels, and reproductive organs. By contracting and relaxing these muscles, Kegels can improve function and provide relief for various pelvic health issues in both men and women.
However, Kegels are just one part of pelvic floor exercise training, and they aren’t always the best fit for everyone. A comprehensive approach includes a thorough assessment with a pelvic floor physiotherapist and often goes beyond Kegels for effective results.
In some cases, like pelvic pain, certain sexual health conditions, or post-birth issues, Kegels can actually make things worse. These problems often come from overly tight pelvic floor muscles. A more holistic approach is needed. This might include lengthening exercises, muscle release, and targeted strengthening.
The key takeaway? There’s much more to pelvic floor exercise training than just Kegels, and a personalized approach with an experienced pelvic floor physiotherapist is essential for optimal results.
Myth: Urinary or fecal incontinence is an inevitable part of getting older.
Fact: Although incontinence becomes more common with age, it is not normal and can often be treated or managed with pelvic floor therapy and lifestyle changes.
Leakage should not be accepted as a normal part of aging. Although aging does increase the risk of incontinence due to factors like weakened pelvic muscles, hormonal changes, medications, and chronic conditions (Goepel et al., 2010), effective treatments are available. These include pelvic floor exercises, bladder training, dietary adjustments, and, in some cases, medical interventions such as surgery, medications, or devices like the Uresta or a pessary. (Goepel et al., 2010).
Pelvic floor therapy is a minimally invasive option that can significantly improve the quality of life for older adults by reducing or even eliminating leakage symptoms (Goepel et al., 2010). In fact, pelvic floor physio is the gold standard treatment for incontinence, rated more effective than surgery. It’s essential to seek help rather than assume incontinence is something to live with. Your quality of life will thank you for it!
Myth: Experiencing pain with sexual activity is normal, especially after childbirth.
Fact: Pain with sexual activity is not normal and can be a sign of underlying pelvic floor issues, which can often be addressed with proper treatment and pelvic floor physiotherapy.
Many women believe that pain during intercourse, especially postpartum, is something they just have to live with. However, while painful sex may be common it is not normal and should be addressed (Tayyeb & Gupta, 2023).
According to Sorensen et al. (2018), pain with sexual activity can be caused by various factors, including:
Pelvic floor physiotherapy can be a valuable treatment for pain with sexual activities. Your pelvic health physio can work with you to:
Pelvic floor physical therapy can identify and treat the underlying causes of pain with sexual activities, leading to more enjoyable sexual experiences.
Myth: Problems with the pelvic floor will always present with clear and noticeable symptoms.
Fact: Pelvic floor dysfunction can sometimes have subtle or unrelated symptoms, such as lower back pain or hip discomfort, and may not always be immediately recognized as a pelvic floor muscle issue.
Pelvic floor muscle dysfunction does not always manifest with obvious symptoms like bladder leakage or pelvic pain. In fact, sometimes the signs can be more subtle, such as persistent lower back pain, hip discomfort (Zhao & Zhao, 2013), or even digestive issues (Wang et al., 2010).
Because these symptoms can be mistaken for other conditions, pelvic floor muscle problems often go undiagnosed. It’s important to consider that your pelvic floor muscles may contribute to your concern when experiencing unexplained pain or discomfort in the lower torso. A thorough assessment by a pelvic health physiotherapist can uncover issues that might otherwise be overlooked, leading to appropriate treatment and relief.
Debunking these common myths is a crucial step toward better understanding and treating pelvic health issues. Moreover, it also brings social awareness about the impacts and importance of your pelvic health. Pelvic health concerns aren’t limited to any gender or age group. Addressing them can significantly improve the quality of life across the lifespan.
If you or someone you know is experiencing pelvic health issues, seek help from a qualified pelvic health physiotherapist. They can assess your specific concerns and provide tailored treatment. Prioritizing pelvic health positively impacts all aspects of your well-being, making it an essential part of your health and self-care routine.
If you have questions relating to your pelvic health, please book an appointment with one of our experienced pelvic health physiotherapists, click here.
~The Bump Team
Bump Physio & Co is a community of health care providers dedicated to changing the way pelvic health and obstetrical services are delivered. Our two clinics locations are Port Moody and Langley BC, where we treat beyond the Bump and welcome clients from all stages and phases of life. Our team has advanced training in Pelvic Health, Orthopedics, Obstetrics, Clinical Pilates, and Active Rehabilitation.
Please follow us along on our socials @bumpphysio.co keep updated on all that is going on and for more information about how the Bump Community can help YOU!
Citations
Bi X, Zhao J, Zhao L, et al. Pelvic floor muscle exercise for chronic low back pain. Journal of International Medical Research. 2013;41(1):146-152. doi:10.1177/0300060513475383
Cho, S. T., & Kim, K. H. (2021). Pelvic floor muscle exercise and training for coping with urinary incontinence. Journal of Exercise Rehabilitation, 17(6), 379-387. https://doi.org/10.12965/jer.2142666.333
Davis, K., & Kumar, D. (2003). Pelvic floor dysfunction: A conceptual framework for collaborative patient-centred care. Journal of Advanced Nursing, 43(6), 555-568. Retrieved from: https://doi.org/10.1046/j.1365-2648.2003.02754.x
Dorey, G., Speakman, M., Feneley, R., Swinkels, A., Dunn, C., & Ewings, P. (2004). Randomised controlled trial of pelvic floor muscle exercises and manometric biofeedback for erectile dysfunction. The British Journal of General Practice, 54(508), 819-825. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1324914/
Goepel, M., Kirschner-Hermanns, R., Welz-Barth, A., Steinwachs, C., & Rübben, H. (2010). Urinary Incontinence in the Elderly: Part 3 of a Series of Articles on Incontinence. Deutsches ÄRzteblatt International, 107(30), 531-536. https://doi.org/10.3238/arztebl.2010.0531
Grimes WR, Stratton M. Pelvic Floor Dysfunction. [Updated 2023 Jun 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK559246/
Lee, B. A., Kim, S. J., Choi, D. K., Kwon, O., Na, H. R., & Cho, S. T. (2017). Effects of Pelvic Floor Muscle Exercise on Urinary Incontinence in Elderly Women With Cognitive Impairment. International Neurourology Journal, 21(4), 295-301. https://doi.org/10.5213/inj.1734956.478
Mayo Clinic. (2008). Kegel exercises for men: Understand the benefits.
Retrieved from: https://www.mayoclinic.org/healthy-lifestyle/mens-health/in-depth/kegel-exercises-for-men/art-20045074
Peinado Molina, R. A., Martínez, A. H., Vázquez, S. M., & Martínez Galiano, J. M. (2023). Influence of pelvic floor disorders on quality of life in women. Frontiers in Public Health, 11. https://doi.org/10.3389/fpubh.2023.1180907
Retrieved from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10629477/
Tayyeb M, Gupta V. Dyspareunia. [Updated 2023 Jun 5]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2024 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562159/
Wang, J. Y., Varma, M. G., Creasman, J. M., Subak, L. L., Brown, J. S., Thom, D. H., & Van Den Eeden, S. K. (2010). Pelvic floor disorders and quality of life in women with self-reported irritable bowel syndrome. Alimentary Pharmacology & Therapeutics, 31(3), 424.
Retrieved from: https://doi.org/10.1111/j.1365-2036.2009.04180.x
Zivkovic V., Lazovic, M., Vlajkovic, M., Slavkovic, A., Jovanovic, Z. (2010). The Role of Pelvic Floor Rehabilitation in the Treatment of Children with Dysfunctional Voiding. Journal of Pediatric Urology, 6.
Retrieved from: https://doi.org/10.1016/j.jpurol.2010.02.126






Meet Everything
Kegel weights were originally developed to provide a more effective and engaging way to perform pelvic floor muscle training. Think of them is as dumbbells for your pelvic floor muscles! Kegel weights, also known as vaginal weights, pelvic floor weights, and vaginal cones come in various shapes and sizes, typically resembling small balls or cones. Ideally, they are made from body-safe materials like silicone or plastic and often come in varying colour-coded sets. Kegel weights are used progressively, starting with a lighter weight and gradually moving to heavier ones as the pelvic floor muscles become stronger.
Kegel weights are inserted into the vagina. Once inserted, the user relies on their pelvic muscles to keep the weight in place during activity. They can be used in various positions, from lying to sitting and standing; progressing from easier to more difficult positions. We want to remind you that these handy conditioning devices are are to be used for your exercises only. Once your exercises are completed, the weight is to be removed. Do not leave Kegel weights in all day. The result? With regular use, stronger pelvic floor muscles. Stronger pelvic floor muscles can be helpful in reducing issues relating to urinary incontinence, pelvic organ prolapse and sexual health. More on that below!
Before we continue…
This post, written from a physiotherapy perspective, aims to be informative for both allied health professionals and individuals interested in learning more about Kegel weights.
Before we dive into the details about Kegel weights, let’s start at the beginning: pelvic floor muscle training.
Traditional Kegel exercises are a method of pelvic floor muscle training designed to help individuals strengthen and tone their pelvic floor muscles. While Kegels can be beneficial on their own, they sometimes lack the sensory feedback necessary for individuals to properly engage their pelvic floor muscles (Herbison & Dean, 2013). This renders the exercise ineffective.
Enter, Kegel weights. Kegel weights provide this feedback, making it easier for users to identify and properly contract their muscles during exercises (Cho & Kim, 2021). These small, weighted devices are designed to be inserted into the vagina to aid in strengthening and retraining the pelvic floor muscles, helping individuals recognize and control their pelvic floor more effectively (Herbison & Dean, 2013).
As Cho & Kim (2021) explain, the pelvic floor is a group of muscles that forms a hammock-like structure at the base of the pelvis. It stretches from the pubic bone at the front to the tailbone at the back and from one sitting bone to the other. These muscles support the pelvic organs, including the bladder, uterus (or prostate in males), and rectum. They also help control bowel and bladder functions and play an important role in sexual function. Keeping the pelvic floor muscles strong and coordinated can alleviate a range of conditions and improve overall pelvic health.
Improved Muscle Awareness
Kegel weights can help individuals better recognize and control their pelvic floor muscles. The sensation of the weight inside the vagina provides immediate feedback, prompting the muscles to contract and hold the weight in place. This awareness is invaluable for performing pelvic floor exercises correctly and effectively.
Enhanced Exercise Adherence
Raise your hand if you need help remembering to do your Kegels?! You’re not alone! As with any exercise routine, maintaining consistency can be challenging. Kegel weights add a “tangible element” (Cho & Kim, 2021) to the exercises, making them more engaging and easier to remember.
Effective Resistance Training
Like any other muscle group, the pelvic floor muscles benefit from resistance training. Kegel weights act as resistance, making the exercises more challenging. As you progress, you can gradually increase your weight, building the strength and endurance in your pelvic floor muscles.
Enhanced Sexual Health
Stronger pelvic floor muscles can enhance sexual sensation and satisfaction by increasing vaginal tone and blood flow to the area. This can lead to more pleasurable experiences during intercourse and more intense orgasms. The resistance provided by Kegel weights helps achieve these benefits may be more effective in strengthening the pelvic floor than Kegel exercises alone.
Improved Bladder Control
Kegel weights can significantly improve conditions like stress incontinence (leakage during activities like coughing or lifting) and urge incontinence (a sudden, intense urge to urinate). Strengthening the pelvic floor muscles with weights can help regain bladder control and reduce the frequency and severity of leaks.
Postpartum Recovery
After childbirth, pelvic floor muscles can be stretched and weakened. As a result, 1 in 3 postpartum individuals experience involuntary bladder leakage (Herbison & Dean, 2013). Using Kegel weights can help new mothers regain muscle strength and improve bladder control. Early intervention with Kegel weights can support a smoother postpartum recovery and prevent long-term pelvic floor issues.
Preventing Pelvic Organ Prolapse
Regular use of Kegel weights can help prevent pelvic organ prolapse, where pelvic organs descend due to weakened support structures. Strengthening the pelvic floor muscles can provide better support for the pelvic organs and reduce the risk of prolapse. In addition, they can also be used as a treatment for mild presentations of Pelvic Organ Prolapse.
Using Kegel weights might feel intimidating but, really, it’s just a few simple steps. That said, following the steps carefully is important to avoid injury or discomfort. We strongly recommend using these tools under the guidance of a pelvic floor physiotherapist rather than on your own.
Prioritize Cleanliness
Before inserting your Kegel weight, ensure that you thoroughly wash your hands and the weight you intend to use, thoroughly with a fragrance-free soap and warm water or a menstrual cup cleanser.
Choose the Right Kegel Weight
Begin with the lightest weight in the set. As your muscles strengthen, you can gradually move to heavier weights.
Insertion
Apply a small amount of water-based lubricant to the weight. Insert it into the vagina in a comfortable, standing or lying down position, similar to inserting a tampon.
Engage Your Muscles
Once the weight is in place, contract your pelvic floor muscles to hold it inside. You should feel your muscles lifting the weight.
Exercise Routine
Exercise routines will be unique based on the individual’s condition and lifestyle. A general routine will begin with short sessions, around 5 minutes, once or twice a day. Gradually increase the duration as your muscles get stronger. Aim for up to 15-20 minutes per session (Herbison & Dean, 2013).
When integrating Kegel weights into your pelvic floor muscle training, it’s important to vary your exercise positions and the speed of contractions to make your routine more dynamic.
Remove and Clean
After your session, remove the weight gently. Clean it with mild soap and warm water, and dry it thoroughly before storing.
For more, check out this excellent instructional video here:
Consistency is Key
Regular use is essential for seeing results. Try to incorporate the exercises into your daily routine.
Listen to Your Body
If you experience pain or discomfort, stop using the weights and consult with a healthcare professional.
Combine with Other Exercises/Physical Therapies
Incorporating other pelvic floor exercises, such as traditional Kegels without weights, can enhance the strengthening effect.
Stay Relaxed
Sometimes this one is easier said than done! Avoid tensing other muscles (like the abdomen or bum) while doing the exercises. Focus on isolating the pelvic floor muscles.
Kegel weights are beneficial for many pelvic floor conditions, yet it’s important to note that they may not be suitable for everyone. Some conditions may be worsened by their use. These include:
Active Infections
Using Kegel weights during an active pelvic infection could exacerbate symptoms or hinder healing.
Recent Pelvic Surgery
Immediately after pelvic surgery, including procedures like a hysterectomy or repair of pelvic organ prolapse, Kegel weights might not be recommended until healing progresses.
Severe Pelvic Pain
Conditions causing severe pelvic pain, such as acute pelvic inflammatory disease or severe endometriosis, may not benefit from Kegel weights until pain is adequately managed.
Uncontrolled Pelvic Floor Spasms
In cases of hypertonic pelvic floor dysfunction where the muscles are overly tense and spasming, Kegel weights could potentially worsen symptoms. If you are experiencing persistent low back or hip pain, please do not use Kegel weights until you have been assessed by a pelvic floor physiotherapist.
Pelvic Organ Prolapse (in certain cases)
While Kegel exercises are often recommended for mild to moderate pelvic organ prolapse, severe cases may require more specialized interventions.
It is vital to consult with a healthcare provider or pelvic floor physiotherapist before starting any pelvic floor exercise regimen, including the use of Kegel weights, to ensure they are appropriate for your specific condition and needs.
Kegel weights, developed as a supplementary treatment to traditional pelvic floor muscle exercises, offer an effective and engaging way to strengthen these key muscles. By providing immediate feedback, enhancing exercise adherence, and acting as a form of resistance training, Kegel weights can help individuals achieve better outcomes in pelvic floor health and overall well-being.
You can shop one of our favourite sets of Kegel weights here. To receive personalized guidance and support regarding Kegel weights, please book an assessment with one of our pelvic floor physiotherapists here.
Bump Physio & Co is a community of health care providers dedicated to changing the way pelvic health and obstetrical services are delivered. Our two clinics locations are Port Moody and Langley BC, where we treat beyond the Bump and welcome clients from all stages and phases of life. Our team has advanced training in Pelvic Health, Orthopedics, Obstetrics, Clinical Pilates, and Active Rehabilitation.
Want to tap into all the pelvic floor expertise the Bump Community has to offer? Follow us on our socials! @bumpphysio.co
Citations
Herbison, G. P., & Dean, N. (2013). Weighted vaginal cones for urinary incontinence. The Cochrane database of systematic reviews, 2013(7), CD002114. https://doi.org/10.1002/14651858.CD002114.pub2
Retrieved from:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7086390
Cho, S. T., & Kim, K. H. (2021). Pelvic floor muscle exercise and training for coping with urinary incontinence. Journal of Exercise Rehabilitation, 17(6), 379-387.
Retrieved from:






Meet Chronic
Pelvic pain is a condition that affects 26% of the world’s female population, yet it remains cloaked in misunderstanding, often going misdiagnosed or untreated (Lamvu et al., 2021). While you may think this pain affects one exclusively in a physical sense, research long supports a strong relationship between pelvic pain and one’s psychological well-being. This relationship is complex, and one worth diving into to help explain not only how they are linked but what we can do to help decrease your pain and improve your quality of life.
Before we continue…
We want to acknowledge that pelvic pain affects people of all genders, even though this post focuses on female pelvic pain. Written from a physiotherapy perspective, this post aims to be valuable for both allied health professionals and individuals coping with persistent pelvic pain. Also note that while we use the term “chronic pelvic pain” during our discussion, we recognize that current literature supports the use of the term “persistent pelvic pain.”
As Lamvu et al. (2021) explain, chronic pelvic pain (CPP) is a persistent pain in the lower abdomen or pelvis that lasts six months or longer, significantly impacting daily life and overall well-being. It can negatively impact your:
You may also experience symptoms indicating issues with your urinary tract, bowel, muscles or gynecological health. Chronic pelvic pain can be non-cyclic, cyclic, or related to your menstrual cycle and intercourse (Lamvu et al., 2021). As this condition can stem from a variety of sources, diagnosis and treatment are complex. Oftentimes, multiple pelvic pain conditions coexist (Lamvu et al., 2021). Common pelvic pain conditions include:
The human body and mind are intricately linked, with each influencing the other in profound ways (Renoir & Gray, 2013). This is especially evident in chronic pain conditions, including pelvic pain. The central nervous system, which includes the brain and spinal cord, plays a crucial role in our perception of pain.
When someone experiences chronic pain, their brain’s pain processing centre can become hypersensitive, leading to an exaggerated pain response (Till et al., 2019). This phenomenon is known as central sensitization (Latremolier & Woolf, 2009). When someone is centrally sensitized, their nervous system goes on what could be called “high alert.” When on “high alert,” any stimulation might be perceived by the central nervous system as dangerous or painful. With repeated stimulation over time, the pain response continues to be amplified.
Beyond the physical symptoms, chronic pelvic pain can often lead to psychological distress. The persistent nature of the pain can contribute to anxiety, depression, and a reduced quality of life (Till et al., 2019). The psychological impact is not simply a derivative of living with chronic pain; the psychological impact can also exacerbate the pain itself (Till et al., 2019). Increased levels of stress and anxiety can trigger or worsen pain through the body’s stress response, which activates the sympathetic nervous system. This system releases stress hormones like cortisol, which can increase inflammation and sensitivity to pain (Till et al., 2019).
Individuals living with persistent pain can get trapped in a negative reinforcing feedback loop where their physical symptoms impact their mental and emotional well-being or vice versa, often amplifying their symptoms. Regardless of which one comes first, the impacts can be similar: increased pain, discomfort, and a decreased quality of life.
According to Till et al. (2019), a multidisciplinary approach to treating pelvic pain is often the most effective. This approach typically includes a combination of medical, psychological, and physical therapies aimed at addressing both the physical, emotional, and psychological aspects of pain (Lamvu et al., 2021).
Medical Interventions
Various medical interventions are often used in treating individuals living with persistent pain. These interventions can include medications to manage pain and inflammation, as well as treatments for underlying conditions such as endometriosis or interstitial cystitis (Lamvu et al., 2021). In some cases, nerve blocks or other interventions may be necessary to provide relief, however, the evidence supporting their use is limited when compared to other treatment modalities (Lamvu et al., 2021).
Psychological Therapies
Psychotherapies, including working with a registered clinical counsellor, can help individuals manage the psychological impact of chronic pain (Lamvu et al., 2021). These therapies can teach coping strategies, reduce stress, and address any underlying trauma or mental health issues.
As a team, we strongly believe in co-treating chronic pain and pelvic pain with the help of a mental health professional for the best results. You can read more about our resident Bump registered clinical counsellor here. Alternatively, you can find a list of additional resources at the bottom of this blog post.
Physiotherapy
Working with a registered physiotherapist who has taken additional training in the treatment of pelvic pain can be extremely beneficial for many individuals living with pelvic pain conditions. Physiotherapy techniques that can help reduce pain and improve overall function (Lamvu et al., 2021) include:
From a physiotherapy management lens, it’s important to find ways to downtrain or calm the nervous system to prevent the body from perceiving any kind of touch, stimulation, or movement as painful. It’s also important for physiotherapists and other medical providers to choose positive or neutral language when working with clients with chronic pain to avoid further catastrophizing and reinforcing a negative treatment outcome.
Lifestyle Modifications
Stress reduction techniques, such as mindfulness, meditation, yoga, and relaxation exercises, can also play a critical role in managing both chronic pain and mental health. Encouraging regular physical activity, a balanced diet, and adequate sleep are also essential components of a comprehensive treatment plan (Till et al., 2019).
Understanding the connection between pelvic pain and mental well-being highlights the need for a holistic view of pain management. Those suffering from pelvic pain are encouraged to discuss their physical, emotional, and mental health openly with their healthcare providers and seek integrated treatment plans that address all of their needs. It’s important to know that each discipline and clinician might impart a different lens and treatment approach to your specific condition. Please know that what’s most valuable is that the treatment approach is best for you!
By acknowledging and addressing the psychological components of chronic pelvic pain, healthcare providers can offer more effective and compassionate care. This approach not only helps alleviate symptoms but also improves the overall well-being and quality of life for those living with pelvic pain (Till et al., 2019).
The relationship between pelvic pain and mental health is a testament to the complex, and wondrous, interplay between mind and body. Recognizing and addressing this connection is crucial for effective treatment and improved outcomes for those struggling with chronic pelvic pain.
If you are dealing with chronic pelvic pain, compassionate help is available. Please book online to seek advice/treatment from one of our experienced pelvic floor physiotherapists or to work with our registered clinical counsellor as we believe their interdisciplinary care goes hand in hand.
Bump Physio & Co is a community of health care providers dedicated to changing the way pelvic health and obstetrical services are delivered. Our two clinics locations are Port Moody and Langley BC, where we treat beyond the Bump and welcome clients from all stages and phases of life. Our team has advanced training in Pelvic Health, Orthopedics, Obstetrics, Clinical Pilates, and Active Rehabilitation.
Please follow us along on our socials @bumpphysio.co keep updated on all that is going on and for more information about how the Bump Community can help YOU!
Resources
International Pelvic Pain Society
Citations
Lamvu, G., Carrillo, J., Ouyang, C., Rapkin A. (2021). Chronic pelvic pain in women. Journal of the American Medical Association, 325(23),2381-2391.Retrieved from:
https://academy.flexwebdiensten.nl/wp-content/uploads/2023/09/Lamvu-2021.pdf
Latremoliere, A., & Woolf, C. J. (2009). Central sensitization: a generator of pain hypersensitivity by central neural plasticity. The journal of pain, 10(9), 895–926. https://doi.org/10.1016/j.jpain.2009.06.012
Retrieved from:
Central Sensitization: A Generator of Pain Hypersensitivity by Central Neural Plasticity – PMC
Renoir, T., Hasebe, K., & Gray, L. (2013). Mind and body: how the health of the body impacts on neuropsychiatry. Frontiers in pharmacology, 4, 158.
Retrieved from:
https://doi.org/10.3389/fphar.2013.00158
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3866391
Till, S. R., As-Sanie, S., & Schrepf, A. (2019). Psychology of Chronic Pelvic Pain: Prevalence, Neurobiological Vulnerabilities, and Treatment. Clinical obstetrics and gynecology, 62(1), 22–36. https://doi.org/10.1097/GRF.0000000000000412
Psychology of Chronic Pelvic Pain: Prevalence, Neurobiological Vulnerabilities, and Treatment – PMC






Meet Endometriosis
Did you know that pelvic health physiotherapists can help treat the symptoms of endometriosis? Currently, endometriosis affects 1/10 people with a uterus in Canada and is severely misunderstood, mis or poorly diagnosed and takes a long time to diagnose. The average time from symptom onset to receiving a diagnosis can range from 6-12 years.
In this post, we are going to review what is endometriosis, its signs and symptoms, how the pelvic floor muscles are involved and provide some insights into how pelvic health physiotherapists can help.
Endometriosis is a condition in which the tissue that normally lines the inside of the uterus (the endometrium) grows outside of the uterus. This can cause inflammation, scarring, and adhesions in the pelvic region, which can lead to pain and other symptoms.
The symptoms of endometriosis can vary from person to person, but they often include:
If you experience any and/ or all of these symptoms, please check in with your primary care medical provider for an assessment.
Did you know that Endometriosis can have a significant impact on your pelvic floor muscles? When the endometrial tissue grows outside of the uterus, it can cause inflammation and scarring in the pelvic region. This can lead to a range of pelvic floor problems, including:
Pelvic health physiotherapists are a great resource and can be a helpful ally on your health care team in navigating endo symptoms. Pelvic health physiotherapists are here to support you in providing education, resources, exercises and manual therapies to alleviate pelvic and abdominal pain, improve bladder and bowel function, hands on myofascial release techniques to the abdomen, hips, low back, glutes, pelvic floor and inner thighs to relieve tension, dry needling or IMS techniques, advocate on your behalf for ongoing therapeutic and medical treatments and providing community referrals to other providers who would be a welcomed addition to your care team.
Many individuals diagnosed with endometriosis can benefit from breath work and pelvic floor muscle lengthening activities. If you are feeling tension or pain in your pelvic floor, here are a few suggestions of exercises to try. When in doubt or if you would like a tailored program to you, a registered pelvic health physiotherapist can help!
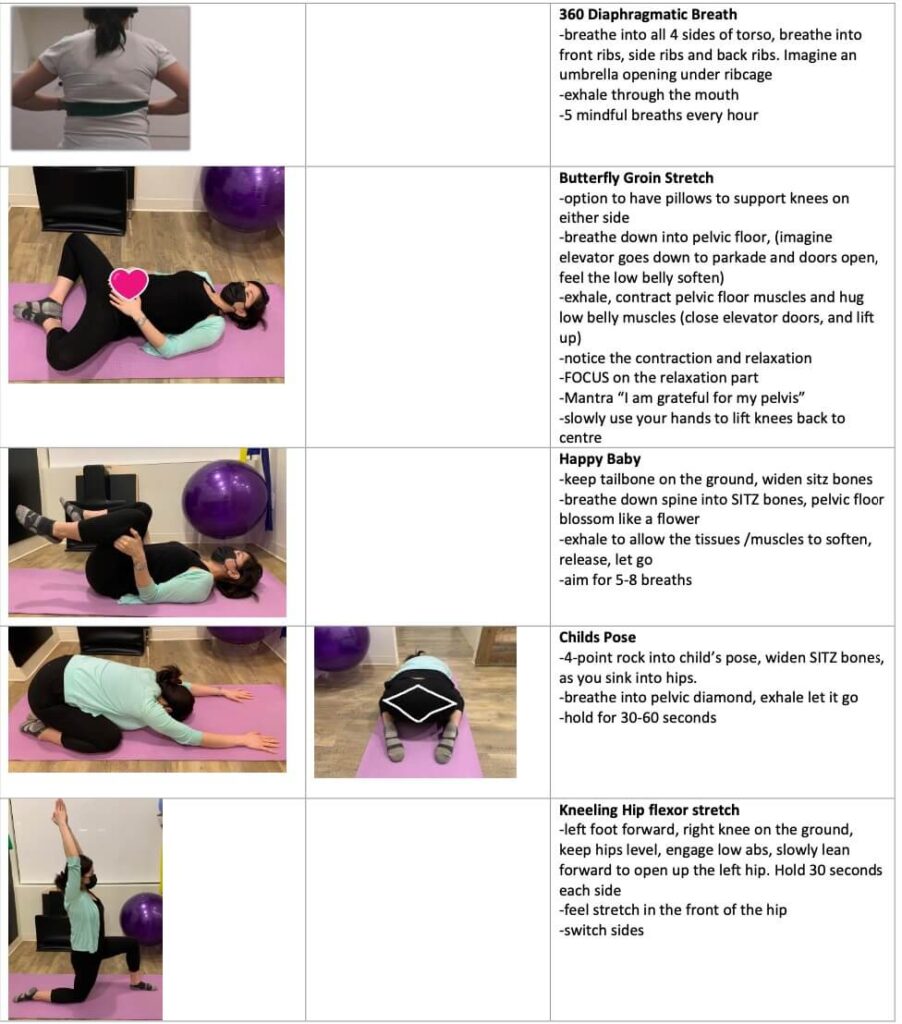

There are also a few products that could be helpful in managing symptoms, including period underwear designed for heavy flows, the Ohnut for pain with receptive intercourse, vaginal dilators or a pelvic wand to decrease pelvic floor muscle tone. If you are curious about how any of these products might be able to help you, please consult with a pelvic health physiotherapist prior to incorporating them into your self care routine.
Endometriosis is a challenging condition to diagnose and treat, which can lead to a significant delay in diagnosis and can impact an individual’s physical and mental health and quality of life. Management of endometriosis requires a multi system, integrated and holistic approach. If you are experiencing symptoms of endometriosis, we encourage you to discuss your concerns with a trusted medical provider.
If you have been diagnosed with Endometriosis and are looking for community connections and resources, here are a few blogs and social media pages to check out.
Instagram pages to follow for connection, information and support!
Questions about Endometriosis and the pelvic floor? Ask us in the comments below.
Lacey Forsyth, MPT
Founder and Registered Physiotherapist at Bump Physio & Co
Bump Physio & Co is a community of health care providers dedicated to changing the way pelvic health and obstetrical services are delivered. Our two clinics locations are Port Moody and Langley BC, where we treat beyond the Bump and welcome clients from all stages and phases of life. Our team has advanced training in Pelvic Health, Orthopedics, Obstetrics, Clinical Pilates, and Active Rehabilitation.
Please follow us along on our socials @bumpphysio.co keep updated on all that is going on and for more information about how the Bump Community can help YOU!
Agarwal SK; Chapron C; Giudice LC, Clinical diagnosis of endometriosis: a call to action. American Journal of Obstetrics & Gynecology; 2019: 354-364.
dos Bispo, A.P.S., Ploger, C., Loureiro, A.F. et al. Assessment of pelvic floor muscles in women with deep endometriosis. Arch Gynecol Obstet 294, 519–523 (2016). https://doi.org/10.1007/s00404-016-4025-x
Gehrich AP, Aseff N, Iglesia CB, Fischer JR, Buller JL. Chronic urinary retention and pelvic floor hypertonicity after surgery for endometriosis: A case series.
Orr NL, Noga H, Williams C. Deep Dyspareunia in Endometriosis: Role of the Bladder and Pelvic Floor. J Sex Med 2018;15:1158-1166.
Vilasagar S, Bougie O, Singh SS. A Practical Guide to the Clinical Evaluation of Endometriosis-Associated Pelvic Pain. The Journal of Minimally Invasive Gynaecology. (2020) 27, 270−279.
http://www.bcwomens.ca/our-services/gynecology/pelvic-pain-endometriosis/





Meet Pelvic
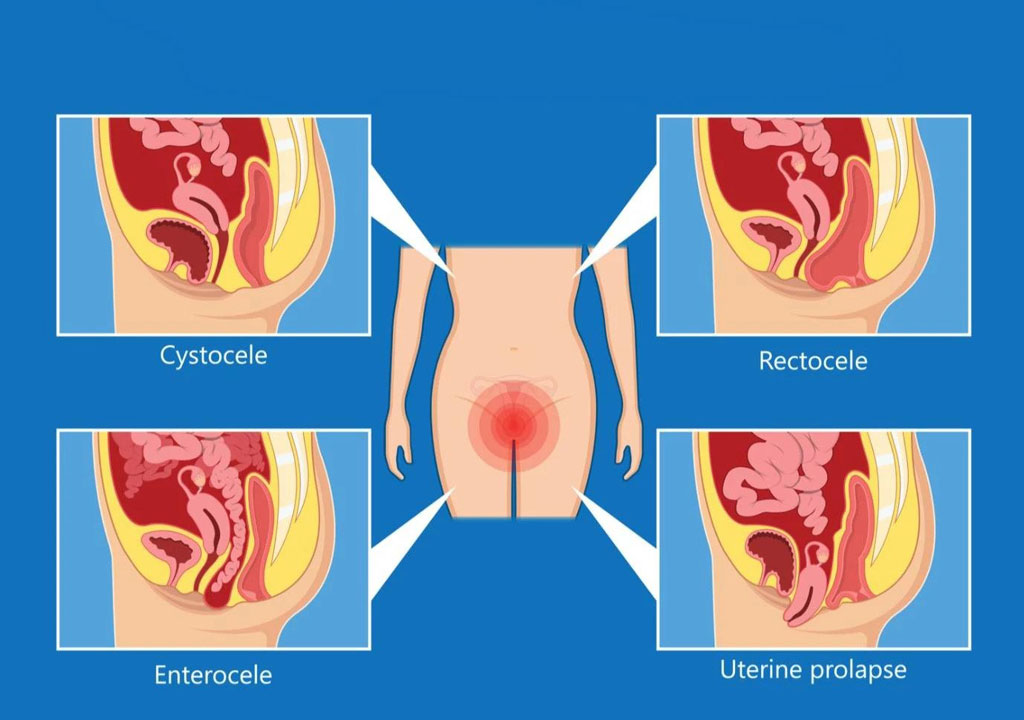
A Pelvic Organ Prolapse (POP) occurs when one or more of the pelvic organs descend toward the bottom of the pelvis from their normal position. Your pelvic organs consist of the bladder/urethra, rectum, and uterus (for biological-cis female populations). There are structures inside the pelvis that help support these organs inside the pelvic cavity; these structures include connective tissue and ligaments that anchor the organs to the bony structure of the pelvis.
The main muscular support of the pelvic organs is your pelvic floor! When injury, dysfunction, or weakening occurs to these supportive tissues, whether it be to the pelvic floor muscles themselves or the ligaments or connective tissues, the organs may drop (or prolapse) down in the pelvis toward the vagina.
This can occur for a variety of reasons, such as pregnancy, childbirth, menopause, chronic coughing, persistent straining for bowel movements, repetitive heavy lifting, weight gain, or any other activities that cause excessive pressure onto your pelvic floor and pelvis. As you can see, there are many reasons you can develop a prolapse, whether you have had children or haven’t!
Many people who develop POP experience symptoms related to their prolapse. However, a portion of people living with POP do not experience any symptoms at all and are considered asymptomatic.
Sometimes reported as the sensation that “something is falling out” of the vagina or rectum. Typically worsened with prolonged standing or walking, impact activities, heavy lifting, and exercise
Leakage, increase urge to empty your bladder, or difficulty completely emptying the bladder

If you suspect you could have a prolapse, always book an evaluation by your family doctor, gynecologist, or pelvic floor physiotherapist. Most prolapses can be addressed successfully with conservative treatment strategies, however surgery may be necessary in some individual cases.
One of the pelvic floor’s main roles is to provide support to the pelvic organs that sit inside the pelvis. When these muscles are lacking strength and not functioning properly, they can cause or contribute to the development of prolapse. Research supports the use of pelvic floor muscle training for treating mild to moderate pelvic organ prolapse, as well as the use of pelvic floor strengthening in alleviating prolapse related symptoms.
This means no straining or pushing to empty your bladder and bowel. Perineal splinting in this case can be helpful to provide counter pressure and support. For exercise, one rule of thumb we always tell our clients is to “blow before you go”. This means exhaling out when you are doing a movement that requires effort and adds load to your body.
This can look like using a stool under your feet when having bowel movements (like a Squatty Potty!), having regular bowel movements, and having adequate fibre and water intake to help with intestinal motility.
This can help penetration feel more comfortable, and reduce friction on the tissue(s) internally.
If you feel any pressure or heaviness in your pelvis, lie on your back with a pillow under your hips and your legs up the wall.
This position allows gravity to bring the pelvic organs further up inside the pelvis, and can help alleviate the feeling of pressure on the bottom of the pelvis.
Savanna Rowe, MPT
🍉 Registered Interim Physiotherapist
Bump Physio & Co is a community of health care providers dedicated to changing the way pelvic health and obstetrical services are delivered. Our two clinics locations are Port Moody and Langley BC, where we treat beyond the Bump and welcome clients from all stages and phases of life! Our team has advanced training in Pelvic Health, Orthopedics, Obstetrics, Clinical Pilates, and Active Rehabilitation.
Please follow us along on our socials @bumpphysio.co to keep updated on all that is going on and for more information about how the Bump Community can help YOU!
Citations
Barber, M.D., Maher, C. Epidemiology and outcome assessment of pelvic organ prolapse. Int Urogynecol J. 2013. 24(11): 1783-1790.
Braekken, I.H., Majida, M., Engh, M.E., Bo, K. Morphological changes after pelvic floor muscle training measured by 3 dimensional ultrasonography: A randomized controlled trial. Obstet Gynecol. 2010. 115(2 Pt 1): 317-324.
Goldstein, S.D., Maxwell, P.J. Rectal prolapse. Clin Colon Rectal Surg. 24(1): 39-45.
Hagen, S., Stark, D., Glazener, C., Sinclair, L., Ramsay, I. A randomized controlled trial of pelvic floor muscle training for stages I and II pelvic organ prolapse. Int Urogynecol J Pelvic Floor Dysfunct. 2009. 20(1): 45-51.
Uzoma, A., Farag, K.A. Vaginal vault prolapse. Obstetrics and Gynecology International. 2009. P. 1-9.
Weintraub, A.Y., Glinter, H., Marcus-Braun, N. Narrative review of the epidemiology, diagnosis, and pathophysiology of pelvic organ prolapse. Int Braz J Urol. 2020. 46(1): 5-14.